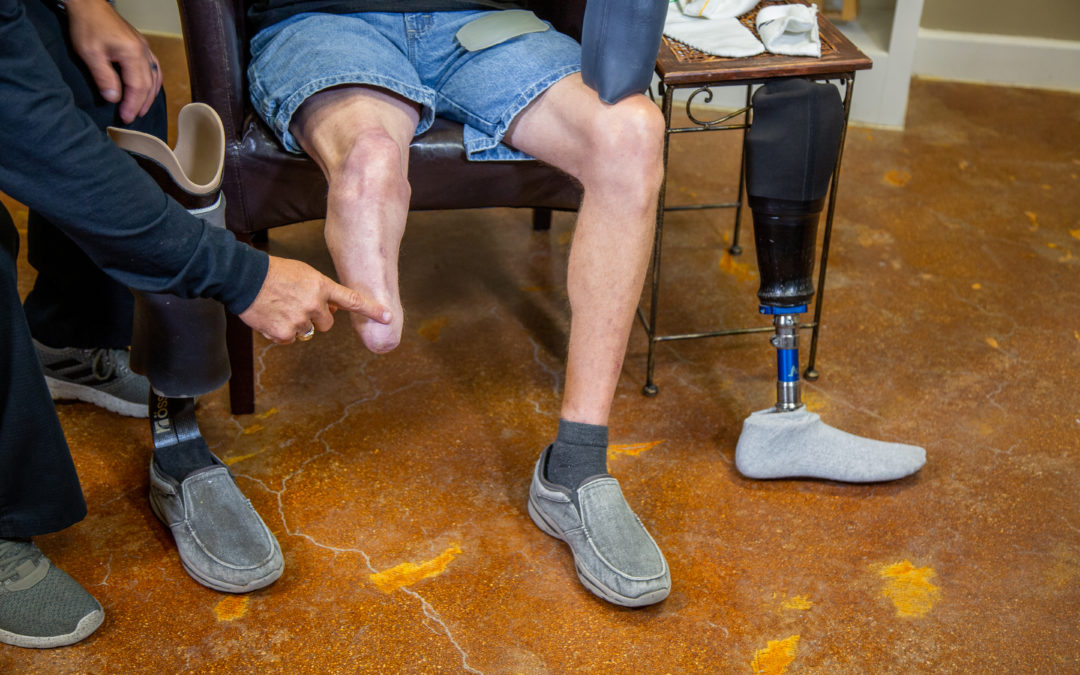
SUMMARY
A lower limb prosthesis refers to a prosthesis that replaces any part of the lower limb to restore the functional and/or cosmetic purpose of the lower limb.
It can be a difficult adjustment when you’ve lost a Introduction to Lower Limb Prosthetic or have had a major lower limb amputation, whether due to injury, disease, or congenital defects.
You may feel like you’ve lost part of your identity and may be facing a long road to recovery. But with the help of a lower limb prosthesis, you can regain your mobility and independence.
This article will discuss all you need to know about lower limb prosthesic.
Overview and Description of Lower Limb Prosthetics
A Lower Limb Prosthetics is an artificial limb that replaces a missing leg or foot. It’s custom-made to fit each individual patient, and it’s designed to restore function and allow the user to live a normal life.
A Lower Limb Prosthetic is usually recommended when a patient has had a lower extremity amputation.
Patients who have had a below-the-knee amputation (BKA) will require a different type of prosthesis than those who have had an above-the-knee amputation (AKA). The type of prosthesis will also vary depending on the level of amputation, as well as the patient’s age, weight, height, and activity level.
Relevance to Clinical Practice
Lower extremity prosthetics are an important part of clinical practice for patients who have had a lower extremity amputation.
There are a number of steps to be taken in order to ensure that the Lower Limb Prosthetic fits properly and functions correctly:
Post-Amputation Process and Prosthetic Evaluation
 Before a patient can be fitted for a prosthesis, they must go through the post-amputation process. This includes surgery to close the wound and various validated patient assessment techniques to determine the best type of prosthesis for each individual.
Before a patient can be fitted for a prosthesis, they must go through the post-amputation process. This includes surgery to close the wound and various validated patient assessment techniques to determine the best type of prosthesis for each individual.
It also involves physical therapy to help the patient regain strength and mobility, and psychological counseling to help the patient adjust to their new body.
Once the post-amputation process is complete, the patient will be evaluated by a prosthetist to see if they are ready for a prosthesis.
Prosthetic Evaluation
Prosthetic evaluation, as we mentioned, involves a number of different assessment techniques to measure the functional ability of the patient and to assess their general health status.
These techniques include:
- Gait analysis: This is a process of observing and measuring a patient’s walking pattern. It helps to identify any problems with the way the patient walks and to determine the best type of prosthesis for them.
- Range of motion and muscle testing: This is a process of measuring the range of motion of the joints and testing the strength of the muscles. It helps to identify any limitations the patient may have and to assess the patient’s maximum attainable functional ability.
- Stump shrinkage: This is a process of measuring the circumference of the residual limb over time. It helps to determine how much the stump will shrink and to ensure that the prosthesis will still fit properly.
Some of the general health status factors that could affect the decision to prescribe a Lower Limb Prosthetic include:
- The patient’s age
- The patient’s weight and height
- The patient’s activity level and lifestyle
- The patient’s mental health status
- The patient’s medical history (e.g., presence of vascular disease)
- The type, location, and level of amputation
Pre-Prosthetic Training
A pre-prosthetic training involves working with a rehabilitation team (physical and occupational therapists) to assess current amputee function. This also includes educating the patient on basic ambulation skills, how to don and doff the prosthesis, and how to care for the skin.
The rehabilitation team will also help the patient understand their new body and learn how to live with their amputation.
Prosthetic Prescription
Once the evaluation and the pre-training are complete, the patient will be ready to be fitted for their prosthesis.
Prosthesis Prescription
A prosthesis prescription is a document that contains all the information about the patient’s amputation, their medical history, and their physical capabilities.
It is used to determine the best type of Lower Limb Prosthetic for the patient and to ensure that the prosthesis is properly fitted.
The prosthesis prescription will include:
- The type of prosthesis: This will be determined by the level of amputation and the patient’s physical capabilities.
- The size of the prosthesis: This will be determined by the stump circumference and the length of the residual limb.
- The weight of the prosthesis: This will be determined by the weight of the patient and the type of prosthesis.
- The activity level of the prosthesis: This will be determined by the patient’s functional status.
Initial Prosthetic Fitting
The initial prosthetic fitting is when the patient is first fitted for their prosthesis. This usually takes place 4-6 weeks after the amputation.
The prosthetist will take measurements of the residual limb and make a plaster cast or positive mold of it. This will be used to create the prosthetic socket.
The prosthetist will also fit the patient for any prosthetic components that are needed, such as a knee joint or foot.
Final Prosthetic Fitting
The final prosthetic fitting is when the patient is fitted for their permanent prosthesis. This usually takes place 3-4 months after the amputation.
The prosthetist will make any adjustments to the fit of the socket and components, and make sure that the prosthesis is functioning properly.
The patient will also be given instructions on how to care for their prosthesis and how to use it properly.
Functional Outcome Measurement
Another part of the patient management strategy is to assess patient satisfaction and measure the functional outcome of the prosthetic device.
Functional outcome measurement tools also include:
- The 6-Minute Walk Test (6MWT)
- The Timed Up and Go Test (TUG)
- The Lower Extremity Functional Scale (LEFS)
In addition to these functional outcome measurement tools, there are also a number of questionnaires that can be used to assess the patient’s satisfaction with their prosthesis. These include:
- The Prosthesis Evaluation Questionnaire (PEQ)
- The Limb Loss and Amputation Satisfaction Scale (LLASS)
- The Prosthetic Profile Questionnaire (PPQ)
The goal of the whole patient management strategy is to provide the best possible care for the patient and to ensure that they are satisfied with their prosthesis.
Poor clinical outcomes can be due to a number of factors, such as:
- An incorrect prosthesis prescription
- A poor fit of the prosthesis
- Poor pre-prosthetic training
- Lack of follow-up care
It is important to note that the success of the prosthesis depends on the patient’s motivation and willingness to participate in their rehabilitation, as well as the care and support that they receive from their prosthetist and rehabilitation team.
Different Lower Limb Prosthetic Components
There are a number of Lower Limb Prosthetic components that can be used to create a Lower Limb Prosthetic:
Prosthetic Socket
The prosthetic socket is the part of the prosthesis that the residual limb fits into. It is made from a plaster cast or positive mold of the residual limb. There are also different kinds of sockets:
- Quadrilateral socket: This is the most common type of socket and it covers the entire residual limb.
- Ischial containment socket: This type of socket has a hole in the back that helps to keep the residual limb in place.
- Subischial socket: This type of socket is shorter than the quadrilateral socket and it does not cover the entire residual limb.
- Hip-disarticulation socket: This type of socket is used for patients who have had a hip disarticulation amputation.
- Thigh-high socket: This type of socket is used for patients who have had a thigh amputation.
- Hemipelvectomy socket: This type of socket is used for patients who have had a hemipelvectomy (half of the pelvis) amputation.
Prosthetic Knee Joint
A prosthetic knee joint is used to provide stability and allow the patient to walk with a natural gait. There are a number of different types of knee joints:
- Single-axis knee joint: This type of joint allows the leg to move forwards and backwards.
- Dual-axis knee joint: This type of joint allows the leg to move forwards and backwards, as well as side to side.
- Multi-axis knee joint: This type of joint allows the leg to move in all directions.
Prosthetic Ankle Joint
Similar to a knee joint, a prosthetic ankle joint is used to provide stability and allow the patient. The kinds of ankle joints are also similar to knee joints: single-axis, dual-axis, and multi-axis.
Prosthetic Foot
A prosthetic foot is used to provide support and allow the patient to walk naturally. There are a number of different types of feet:
- Solid ankle-cushioned heel (SACH) foot: This type of foot is the simplest and most common. It is made from a solid piece of plastic and has a cushion at the heel.
- Pylon foot: This type of foot is made from a metal rod (pylon) that is attached to the ankle.
- Pyramid foot: This type of foot is made from a metal rod that is attached to the ankle and has a pyramid shape at the bottom.
Other Components
Other components can also be attached to the distal residual limb depending on the needs of the patient. These include:
- Ankle-foot orthosis (AFO): This is a supportive device that is worn around the ankle and foot.
- Knee orthosis (KO): This is a supportive device that is worn around the knee.
- Hip spica: This is a type of supportive device that is worn around the hip and waist.
Different Types of Lower Limb Prosthetic
As we previously mentioned, there are a number of types of Lower Limb Prosthetic, each designed for a specific type of amputation:
Partial Foot Prostheses
These are used for patients who have had a partial foot amputation. This type of prosthesis includes a toe filler and covers the entire foot.
Syme’s Prostheses
These are used for patients who have had a Syme’s amputation (amputation through the ankle joint). This type of prosthesis includes a foot and ankle joint.
Transtibial (Below Knee) and Transfemoral (Above Knee) Prostheses
These are used for patients who have had a transtibial amputation (below knee) or a transfemoral amputation (above knee). This type of prosthesis includes a knee joint, ankle joint, and foot.
In some cases, a transtibial or transfemoral suspension is also used. This is a type of harness that goes around the thigh and helps to keep the prosthesis in place.
Disarticulation Prostheses
These are used for patients who have had a knee, ankle, or hip disarticulation amputation. This type of prosthesis includes a knee joint, ankle joint, and foot.
Thigh-High Prostheses
These are used for patients who have had a thigh amputation. Similar to other types of prostheses, this type also includes a knee joint, ankle joint, and foot.
Hemipelvectomy Prostheses
These are used for patients who have had a hemipelvectomy (half of the pelvis) amputation. This kind of prosthesis requires a special socket that covers the entire residual limb. The prosthesis also includes a knee joint, ankle joint, and foot.
Transmetatarsal Amputation Prosthesis
These are used for patients who have had a transmetatarsal amputation (amputation through the metatarsals, the bones in the foot). This type of prosthesis covers the entire foot and includes a toe filler.
Cutting Edge Techniques and Emerging Issues with Prosthetic Devices
In recent years, there have been a number of advances in prosthetic technology. These advances have made it possible for patients to have more natural movement and control over their prosthetic devices.
Prosthetic Technology and Considerations
One of the most cutting-edge advances in prosthetic technology is the development of myoelectric prostheses. These devices use sensors that are placed on the skin to detect the electrical signals that are produced when the muscles contract. This information is then used to control the movement of the prosthesis.
The genium microprocessor knee, for example, is a myoelectric prosthesis that can be used for patients who have had a transtibial amputation. This device is able to provide a number of different features, including 3D motion and improved angle pivot and knee lock.
The C-Leg microprocessor knee is another myoelectric prosthesis that is designed for patients who have had a transfemoral amputation. This device is able to provide a number of features, including stance control, automatic step-length adjustment, and swing phase control.
Future Directions
As technology in the medical field continues to advance, there is a good chance that prosthetic devices will continue to become more advanced. Some of the things that are currently being developed are:
3D printing of prosthetic devices
This could potentially allow for the creation of custom-made prosthetic devices that are specifically designed for each individual patient.
Bionic prostheses
These are devices that are designed to mimic the function of a real limb. They often make use of sensors and motors to provide patients with a more natural range of motion.
The Cambridge Bioaugmentation Systems (CBAS) is one example of a bionic prosthesis that is currently being developed.
Implantable devices
These are devices that are surgically implanted into the body and are then able to provide patients with Lower Limb Prosthetic that are controlled by the nervous system.
Gaps in Knowledge
Despite all the technological advances in prosthetics, evidence gaps exist related to the outcomes of using these devices. In particular, more research is needed to assess:
- The long-term effects of using myoelectric devices
- The long-term effects of using bionic devices
- The long-term effects of using implantable devices
In addition, there is a need for more research on the psychological effects of using prosthetic devices. This includes studies that assess issues such as body image, self-esteem, and quality of life.
Prosthetic Leg Technology Is Always Evolving
There are always new developments in lower limb prosthetic technology, such as microprocessor-driven and activity-specific components.
Microprocessor joints feature computer chips and sensors to provide a more natural gait. They may even have different modes for walking on flat surfaces or up and down the stairs.
There are also specialized prosthetic legs for different activities, such as running, showering or swimming, which you can switch to as needed. In some cases, your everyday lower limb prosthetic can be modified by your prosthetist to serve different purposes.
Osseointegration surgery is another option. This procedure involves the insertion of a metal implant directly into the bone, so there is no need for a socket. The prosthetic leg then attaches directly to that implant. While this procedure is not right for everyone and is still under study, it can provide improved range of motion and sensory perception.
It’s important to remember that you’re not alone in navigating the many different lower limb prosthetic options. Your care team will help you weigh the pros and cons of each and decide on the ideal prosthetic leg that matches your lifestyle.
Alltech Prosthetics: Your Partner in Lower Extremity Prosthetic Care
At Alltech Prosthetics, we are dedicated to providing our patients with the best possible care. We offer a wide range of services, including lower extremity prosthetic care. We are also up-to-date on the latest advances in prosthetic technology and can provide our patients with the most cutting-edge devices.
If you or a loved one are in need of lower limb prosthetic care, contact us today to schedule a consultation. We will work with you to create a treatment plan that meets your unique needs and goals.
FAQ
What are the considerations for choosing a prosthetic device?
The type of prosthetic device that is chosen will depend on a number of factors, including the level of amputation, patient characteristics such as age and activity level, and the preference of the patient.
What are the risks of using a prosthetic device?
There are a number of risks that are associated with using prosthetic devices, including infection, skin breakdown, and stump soreness. In addition, there is a risk of developing phantom limb pain. This is a type of pain that is felt in the limb that has been amputated.
How much does a lower limb prosthesis typically cost?
The cost of a lower limb prosthesis can vary depending on the type of device that is chosen. For example, a transtibial prosthesis can cost anywhere from $5,000 to $10,000. A transfemoral prosthesis can cost anywhere from $8,000 to $30,000.
The costs will also depend on the insurance coverage that is available and the Medicare functional classification level that is assigned to the patient. The beneficiary’s past medical history is also considered when determining the costs.
What is a Medicare functional classification level?
There are five different Medicare functional classification levels for lower limb prosthetics. They are as follows:
- K0 – The patient does not use a prosthetic device and does not have a residual limb.
- K1 – The patient uses a prosthetic device on a limited basis.
- K2 – The patient uses a prosthetic device on a regular basis.
- K3 – The patient uses a prosthetic device and has significant functional limitations.
- K4 – The patient uses a prosthetic device and has the ability to ambulate without assistive devices.
Can you wear a lower limb prosthesis all day?
It is typically recommended that patients only wear their Lower Limb Prosthetic for a few hours at a time. This is to allow the skin to breathe and prevent the development of sores.
How do you train an amputee?
There are a number of different ways that amputees can be trained to use their lower limb prosthetic devices. This includes physical therapy, occupational therapy, and prosthetist-led training sessions.
Support system training is also important for amputees. This type of training teaches patients how to properly care for their prosthetic devices and how to troubleshoot any problems that may arise.
What kind of physical therapy is recommended for lower limb amputees?
The type of physical therapy that is recommended for lower limb amputees will depend on the level of amputation. For example, patients who have undergone a below-knee amputation will typically need to focus on regaining range of motion and strength in the knee and ankle.
In general, one of the main goals is to promote prosthetic ambulation. This means teaching patients how to walk with their new devices. Balance and coordination exercises are also often included in physical therapy plans.
How do you care for an amputated limb?
With limb loss, it is important to keep the amputated limb clean and dry. The stump should also be inspected regularly for any signs of infection, skin breakdown, or soreness.
It is also important to follow the instructions of the prosthetist on how to properly care for the prosthetic device. This includes cleaning the device on a regular basis and checking for any loose components.